Epidural Risks In Labor: What To Know Before You Decide
Understand the potential side effects of epidurals during childbirth, from common issues to rare complications, to make informed decisions.
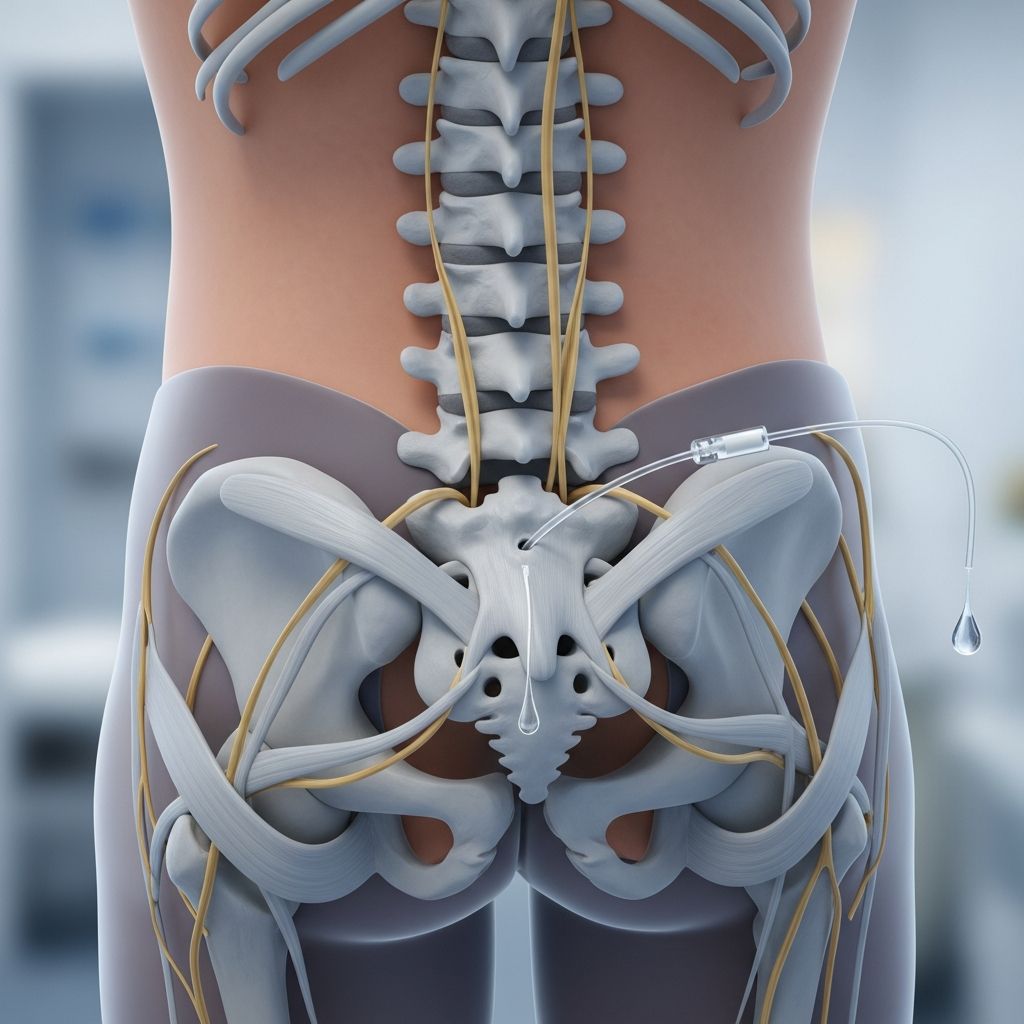
Epidural Risks in Labor: What to Know
Epidural analgesia remains one of the most popular methods for managing pain during childbirth, offering significant relief to many women in labor. However, like any medical intervention, it carries potential risks and side effects that expectant mothers should understand before deciding. This article delves into the common and less common complications associated with epidurals, drawing from clinical studies and expert insights to provide a balanced view.
Understanding Epidural Analgesia Basics
An epidural involves injecting anesthetic medication into the epidural space around the spinal cord to block pain signals from the lower body. Administered typically in active labor, it allows women to remain awake and participate in the birthing process while minimizing discomfort. Despite its effectiveness, the procedure requires precise placement by an anesthesiologist and continuous monitoring.
While epidurals do not cross the placenta in significant amounts to harm the baby directly, they can indirectly affect both mother and fetus through physiological changes such as alterations in blood pressure and uterine blood flow.
Common Immediate Side Effects
Most women experience temporary effects that resolve after delivery. These include:
- Maternal hypotension: A drop in blood pressure occurs in up to 36% of cases, often requiring fluids or medications like vasopressors to correct.
- Numbness and heaviness: Legs may feel heavy or tingly, limiting mobility during labor.
- Itchiness: Pruritus from opioid additives affects many users but is usually mild and treatable with antihistamines.
- Difficulty urinating: The numbing effect can impair bladder function, sometimes necessitating a catheter.
These effects are manageable in hospital settings with close monitoring of vital signs for both mother and baby.
Fetal Heart Rate Changes: A Key Concern
One of the most studied side effects involves transient alterations in fetal heart rate (FHR). Research shows that 11-14% of women experience worsening FHR categories within 60 minutes post-epidural, independent of maternal blood pressure changes.
A study of 439 laboring women found that severe FHR decelerations were linked to a higher cesarean delivery (CD) rate, with logistic regression confirming this association after controlling for confounders like cervical dilation. French data echoed this, noting higher CD rates (21.4% vs. 9.6%) and lower umbilical artery pH in cases with FHR anomalies post-epidural.
| Factor | Impact on CD Risk | P-value |
|---|---|---|
| Cervical dilation at epidural | Increased if less dilated | P=0.03 |
| Labor duration post-epidural | Prolonged increases risk | P<0.001 |
| Worsening FHR within 60 min | Strong independent link | P=0.01 |
This table summarizes key predictors from a cohort study, highlighting how epidural timing and fetal responses influence delivery outcomes.
Links to Prolonged Labor and Cesarean Rates
Epidurals can extend the first stage of labor and increase the need for oxytocin augmentation. Cohort studies, unlike smaller RCTs, detect higher emergency CD risks due to fetal compromise in epidural users.
In one analysis, women requiring CD had higher BMI, less dilation at epidural placement, longer post-epidural labor, and more severe reactions. Mediation analysis revealed direct and indirect paths from these factors to CD, emphasizing vigilant FHR monitoring.
Rare but Serious Complications
Though uncommon, severe risks warrant discussion:
- Post-dural puncture headache: Occurs if the dura is pierced, causing severe headache in 1-2% of cases, treatable with blood patches.
- Infection or hematoma: Rare spinal infections or blood clots can lead to nerve compression; incidence is under 1:10,000.
- Nerve damage: Permanent injury is exceedingly rare, affecting fewer than 1 in 1,000.
- Failed block: Inadequate pain relief may require repositioning.
Apgar scores and NICU admissions remain unaffected, indicating good neonatal outcomes despite maternal challenges.
Long-Term Considerations
Concerns about chronic back pain or numbness persist, but evidence shows no increased long-term risk compared to non-epidural births. Some women report lingering soreness at the insertion site, but this typically resolves.
For fetuses with pre-existing uteroplacental issues, epidurals may exacerbate hypoxia, prompting caution in non-reassuring FHR cases.
Strategies to Minimize Risks
To optimize safety:
- Place epidurals during adequate cervical dilation (4-5 cm) to reduce labor prolongation.
- Monitor FHR closely post-administration, especially in the first hour.
- Use combined spinal-epidural (CSE) judiciously, noting higher bradycardia risk but no CD impact.
- Employ vasopressors promptly for hypotension.
- Consider maternal positioning (side-lying) to maintain placental perfusion.
Multidisciplinary care involving obstetricians, anesthesiologists, and midwives enhances outcomes.
Comparing Epidural to Alternatives
| Method | Pain Relief | Risks | Mobility |
|---|---|---|---|
| Epidural | Excellent | Hypotension, FHR changes | Limited |
| Opioids (IV) | Moderate | Nausea, sedation | Preserved |
| Nitrous Oxide | Mild | Minimal | Full |
| Non-Pharmacologic | Variable | None | Full |
Epidurals outperform opioids in pain control without raising severe perineal tears or postpartum depression risks.
Frequently Asked Questions (FAQs)
Does an epidural increase cesarean section chances?
Studies show an association via FHR changes and prolonged labor, but not causation in all cases. Risk rises with early placement or complications.
Will an epidural harm my baby?
No direct harm; neonatal outcomes like Apgars are comparable. Indirect effects from maternal hypotension are monitored and treated.
How long do side effects last?
Most resolve within hours post-delivery; headaches may persist days but are treatable.
Can I still push with an epidural?
Yes, though leg weakness may require assistance. Dosing adjustments aid pushing.
Who should avoid epidurals?
Those with bleeding disorders, spinal issues, or infection at the site. Discuss with your provider.
Making an Informed Choice
Weighing benefits against risks is personal. Discuss with your healthcare team, considering labor stage, health history, and preferences. Advances in monitoring continue to improve safety profiles.
References
- Side effects from epidural analgesia in laboring women and risk of cesarean delivery — PMC/NCBI. 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC10820310/
- Complications of Epidural Analgesia During Labor — American Academy of Family Physicians (AAFP). 1998-11-15. https://www.aafp.org/pubs/afp/issues/1998/1115/p1743.html
- Epidural Side Effects Long Term, In Pregnancy, Risks, & More — Milestone Scientific. Accessed 2026. https://www.milestonescientific.com/epidural-side-effects-long-term
- Epidurals During Childbirth: What Women Should Know — Yale Medicine. Accessed 2026. https://www.yalemedicine.org/news/epidural-anesthesia
- Epidural during Labor for Pain Management — Evidence Based Birth. Accessed 2026. https://evidencebasedbirth.com/epidural-during-labor-pain-management/
- Epidural: What It Is, Side Effects, Risks & Procedure — Cleveland Clinic. Accessed 2026. https://my.clevelandclinic.org/health/treatments/21896-epidural
Read full bio of Sneha Tete












