Surviving Severe Diaper Rash: A Practical Parent’s Guide
Learn how to recognize, soothe, and prevent even the most stubborn diaper rashes with practical, evidence-based strategies.
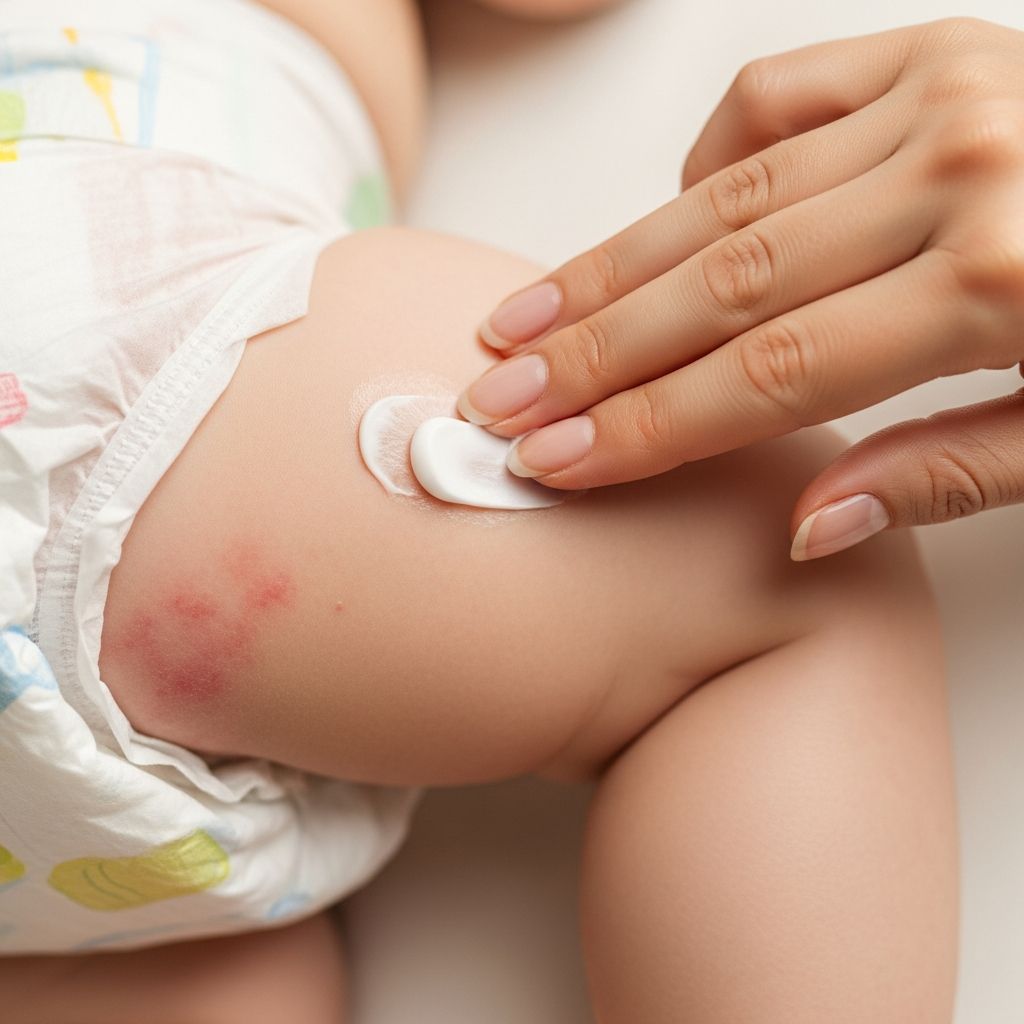
Few things rattle new parents like a baby who screams in pain at every diaper change. Mild diaper rash is common and usually clears quickly, but sometimes it turns into a red, angry, stubborn flare that seems to get worse no matter what you do. This guide explains what’s happening on your baby’s skin, which treatments actually help, and how to know when it is time to see the pediatrician.
Understanding Diaper Rash: More Than Just Red Skin
Diaper rash (also called diaper dermatitis) is irritation and inflammation of the skin in the area covered by a diaper. It can range from faint pink patches to raw, bleeding skin that makes your baby cry with every touch. Though frightening to look at, most cases respond to simple care when you understand the underlying causes.
Common Triggers Behind Diaper Rash
Several factors usually stack together to create a rash, especially in severe cases:
- Prolonged moisture from urine and stool that sits on the skin and breaks down its protective barrier.
- Friction from snug diapers or frequent wiping that rubs and irritates delicate skin.
- Skin contact with stool, especially during diarrhea or frequent bowel movements.
- Changes in diet, such as starting solids, which can make stool more irritating.
- Yeast (candida) overgrowth in warm, damp folds of skin, sometimes after antibiotic use.
- Allergic or irritant reactions to wipes, soaps, creams, or diaper materials.
Newborns and young infants are especially prone because their skin barrier is thinner and less mature than older children’s skin, making it more vulnerable to moisture and friction.
Types of Diaper Rash You Might See
| Type | What It Looks Like | Key Clues |
|---|---|---|
| Irritant diaper rash | Red, inflamed skin on the buttocks, genitals, and inner thighs. | Often spares skin folds; linked to prolonged contact with urine or stool. |
| Yeast (candida) rash | Bright red, slightly raised patches with smaller “satellite” spots. | Common in skin folds and after antibiotics; may not improve with standard barrier creams. |
| Allergic/irritant contact rash | Redness or bumps in areas that touch a specific product. | Appears after new wipes, soap, detergent, or diaper brand. |
Recognizing When a Rash Is Truly “Severe”
Most mild rashes fade within a few days of gentle care. A rash moves into the “severe” category when you see:
- Extensive redness that covers nearly the entire diaper area or spreads down the thighs.
- Open sores, bleeding, or oozing of fluid.
- Thick, sharply defined red patches with smaller red bumps or pustules around the edges (classic for yeast).
- Significant pain—your baby cries or stiffens whenever you wipe, sit them, or lower them into the bath.
- No improvement after 2–3 days of meticulous home treatment.
- Fever, pus, yellow crusts, or spreading redness, which can signal bacterial infection.
If you notice any of these, especially fever or spreading redness, call your pediatrician promptly for guidance.
Step-by-Step Home Care for Bad Diaper Rash
The core of diaper rash treatment is simple: keep the area as clean, dry, and protected as possible while the skin repairs itself.
1. Change Diapers More Often Than Usual
- Check the diaper frequently and change it as soon as it is wet or soiled—even overnight, if the rash is severe.
- During diarrhea or frequent stools, be prepared for many extra changes to limit contact time with stool.
2. Rethink How You Clean the Skin
When the skin is raw, every wipe can feel like sandpaper. To minimize trauma:
- Use warm water and a soft washcloth or cotton pads instead of standard wipes whenever possible.
- If you use wipes, choose alcohol-free, fragrance-free products designed for sensitive skin.
- Pat, do not rub. Dab gently to remove stool and urine; avoid vigorous scrubbing.
- For very painful rashes, you can gently rinse the area with water from a squeeze bottle and allow it to drip dry before applying any cream.
3. Embrace Diaper-Free Air Time
Air is one of the most powerful (and underrated) treatments. Health organizations consistently recommend giving the skin time uncovered by a diaper whenever you can.
- Lay your baby on a waterproof pad or towel and let them play without a diaper for short periods throughout the day.
- Even 10–15 minutes several times per day can significantly reduce moisture exposure.
- Aim for loose clothing or no clothing over the affected area to maximize airflow.
4. Use a Thick, Effective Barrier Layer
Barrier creams protect the skin from further urine and stool contact while it recovers. Pediatric sources commonly recommend:
- Plain petrolatum (petroleum jelly) or thick pastes with zinc oxide as primary ingredients.
- Applying a thick, visible layer—think “frosting,” not lotion—at every diaper change, especially at bedtime.
- Not fully scrubbing off the previous layer if it’s still mostly clean; gently blot, then reapply on top to avoid unnecessary rubbing.
These products do not heal the skin directly; instead, they shield it from irritants so that the body can repair the barrier underneath.
5. Choose Diapers and Clothing That Reduce Friction
- Use diapers that are slightly looser rather than tight-fitting to minimize chafing and allow airflow.
- Avoid plastic pants or diaper covers that trap heat and moisture.
- Dress your baby in soft, breathable fabrics like cotton and avoid rough seams over the irritated area.
When Home Care Is Not Enough: Medical Treatments
Sometimes, a rash is too severe or complicated to manage with home care alone. Pediatric guidelines outline several medical options your clinician might recommend based on the type of rash.
Mild Topical Steroids for Intense Inflammation
For very inflamed, painful skin that does not improve after a couple of days of careful home care, a pediatrician may prescribe or recommend a low-strength hydrocortisone cream (0.5%–1%) for a short course, typically 3–5 days.
- These creams reduce redness and swelling, making the skin more comfortable.
- They must be used exactly as directed—overuse can thin the skin, especially in babies.
Antifungal Creams for Yeast Diaper Rash
If your pediatrician suspects a yeast (candida) infection—especially with bright red patches in the folds and small satellite spots—they may add a topical antifungal cream or ointment.
- These medications target the fungus directly and are applied usually twice daily underneath a barrier cream.
- A rash that worsens or does not improve with standard barrier care may need this kind of treatment.
Antibiotics for Bacterial Infection
Bacterial infection is less common but more serious. It may cause:
- Yellow crusts or scabs
- Pus-filled bumps
- Spreading warmth and redness beyond the diaper area
- Fever or your baby appearing generally unwell
In these cases, a doctor may prescribe topical or oral antibiotics. Do not attempt to treat suspected bacterial infections at home without medical guidance.
Daily Habits to Prevent Future Diaper Rash
Once you have survived a severe episode, prevention becomes a top priority. Fortunately, the same measures that heal rashes can help keep them from returning.
Everyday Prevention Checklist
- Frequent diaper changes: Do not let diapers remain on once they are wet or soiled.
- Gentle cleansing: Use mild, fragrance-free cleansers and avoid harsh wipes or soaps.
- Routine barrier application: Apply a thin layer of zinc oxide or petrolatum at bedtime or whenever you expect longer stretches between changes.
- Regular diaper-free time: Build short “air breaks” into your baby’s day.
- Careful product choices: Introduce new wipes, creams, or detergents one at a time so you can spot potential irritants.
Special Situations That Need Extra Attention
- Antibiotic use: Babies taking antibiotics, or those whose breastfeeding parents are on antibiotics, have a higher risk of yeast diaper rash; consider being more vigilant with changes and calling early if you see a bright red, spotty rash.
- Diarrhea: Increase diaper checks and use extra-thick barrier layers to protect against frequent stool contact.
- Starting solids: New foods can briefly change stool acidity and frequency; monitor your baby’s skin closely during transitions.
Frequently Asked Questions (FAQs)
Q: How long should it take for a diaper rash to improve?
A: Mild diaper rash often improves within 2–3 days of frequent changes, gentle cleansing, and a thick barrier cream, and typically resolves within about a week. If you see no improvement after several days of careful home care, or if the rash worsens, contact your pediatrician.
Q: When should I call the doctor about diaper rash?
A: Call promptly if your baby has fever, blisters, pus, spreading redness, or seems very ill, or if the rash is extremely painful or not better after a few days of home treatment. Also call if you suspect yeast or if your baby is on antibiotics and the rash looks bright red with small satellite spots.
Q: Are cloth diapers or disposable diapers better for preventing rash?
A: Both cloth and disposable diapers can be used successfully. Disposable diapers that wick moisture away from the skin may reduce some types of rash, while cloth requires more frequent changes but allows control over materials and detergents. Regardless of diaper type, the key is frequent changes, gentle cleaning, and regular barrier use.
Q: Can I use cornstarch or talc powder on a bad diaper rash?
A: Current pediatric guidance generally discourages talc powders because of inhalation risks. Cornstarch is sometimes used, but it can be messy and may not be appropriate if a yeast infection is present. Discuss powders with your pediatrician before using them, especially in severe rashes.
Q: How can I tell if my baby’s rash is caused by an allergy to wipes or diapers?
A: Allergic or irritant contact rashes often match the area of skin that touches the product—for example, only where wipes are used or where the diaper’s elastic sits—and may appear shortly after switching brands. If you suspect this, stop using the new product, switch to fragrance-free, dye-free options, and talk with your pediatrician if the rash persists.
Q: Is bathing every day helpful or harmful during a flare?
A: Gentle daily baths with warm water and a mild, fragrance-free cleanser can help keep the area clean while the rash heals. Pat the skin dry carefully afterward and apply a thick barrier cream before putting on a diaper.
References
- Preventing and Treating Diaper Rash — Ann & Robert H. Lurie Children’s Hospital of Chicago. 2022-05-05. https://www.luriechildrens.org/en/blog/preventing-and-treating-diaper-rash/
- Diaper Dermatitis (Diaper Rash) — Nationwide Children’s Hospital. 2021-08-01. https://www.nationwidechildrens.org/conditions/diaper-dermatitis-diaper-rash
- Diaper Rash: Symptoms, Causes & Treatment — Cleveland Clinic. 2023-06-27. https://my.clevelandclinic.org/health/diseases/11037-diaper-rash-diaper-dermatitis
- Diaper Rash – Symptoms & Causes — Mayo Clinic. 2023-02-24. https://www.mayoclinic.org/diseases-conditions/diaper-rash/symptoms-causes/syc-20371636
- Diaper Rash – Diagnosis & Treatment — Mayo Clinic. 2023-02-24. https://www.mayoclinic.org/diseases-conditions/diaper-rash/diagnosis-treatment/drc-20371641
- Diaper Rash — Seattle Children’s Hospital. 2022-10-10. https://www.seattlechildrens.org/conditions/a-z/diaper-rash/
- Common Diaper Rashes & Treatments — American Academy of Pediatrics / HealthyChildren.org. 2020-06-01. https://www.healthychildren.org/English/ages-stages/baby/diapers-clothing/Pages/Diaper-Rash.aspx
Read full bio of Sneha Tete










